When your loved one is ready to leave the hospital, you might feel relief mixed with worry. The transition from hospital to home involves many moving parts, and families often wonder who handles what during this change.
That’s why PalAssist offers free phone support from registered nurses who understand these transitions and can answer your questions any time. With the right guidance, coordinating care between hospital and home doesn’t have to feel overwhelming.
This article covers how Palliative Care Queensland Health coordinates hospital discharge, how teams share information, and what equipment and medications you’ll need at home. You’ll also learn when to reach out for support during the process.
What Does “Care Coordination” Mean in Palliative Care Queensland Health?
Care coordination brings hospital doctors, community nurses, GPs, and specialists onto the same page. They share medical information, agree on treatment plans, and communicate regularly so the person doesn’t experience gaps in care during the transition home.

This coordination focuses on quality of life by addressing:
- Physical symptoms that need ongoing relief
- Emotional needs, if distress or anxiety arises
- Spiritual concerns to honour beliefs and values
- Practical matters like equipment or referrals
When these services link properly, you won’t need to repeat the same medical history to every new person involved in their care.
Who Handles the Transition Between Hospital and Home?
Several different health professionals, including nurses and palliative care specialists, work together to manage the move from hospital to home. Each team handles a specific part of the coordination process.
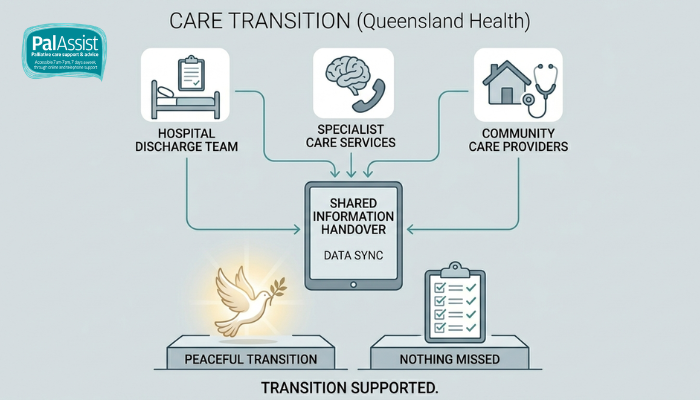
So let’s break down who does what:
Your Hospital Discharge Team
Your hospital discharge team takes care of all the planning work so you can focus on helping your family member. For example:
- Discharge nurses organise medications, equipment, and home care appointments before discharge happens.
- Social workers arrange community support services and answer questions about financial assistance programs.
- Doctors provide written care instructions and emergency contact details for your GP.
Together, they make sure nothing gets missed before you leave the hospital.
Community Palliative Care Providers
Community care providers are nurses and allied health professionals who visit your home after being discharged. In our experience supporting Queensland families, these providers coordinate with hospital specialists to continue the same level of care after discharge.
Worth Noting: Community nurses visit your home regularly to monitor symptoms and adjust treatment plans. You can reach them any time for urgent symptom management advice.
Specialist Palliative Care Services
Sometimes you need extra help from specialists who handle complex symptoms or difficult medical situations. And that’s the main role of specialist palliative care teams. They manage symptoms that require expert knowledge beyond general care. Plus, they provide telephone consultations and home visits for children with paediatric care needs.
Specialists also guide your family through difficult decisions during the dying process, especially when illnesses reach an advanced stage (which gives families peace during uncertain times).
Planning Your Loved One’s Move Home
You might be thinking the hospital discharge process sounds like a lot to organise. But it doesn’t have to be. If you plan through each step, most moves go smoothly without last-minute stress.
And if you’re wondering where to even start, just print out the checklist below, grab a pencil, and tick off items as you complete them.
Hospital to Home Transition Checklist
| Task | ✓ |
| Discharge summary received from the hospital | ☐ |
| Updated medication list with dosages | ☐ |
| Medical equipment ordered, and delivery confirmed | ☐ |
| GP notified of discharge and care plan | ☐ |
| Emergency contact numbers saved | ☐ |
| Follow-up appointments scheduled | ☐ |
| Home assessment completed (if needed) | ☐ |
PalAssist recommends starting discharge planning early so medical equipment arrives before your loved one comes home. Beyond that, request a home visit from community nurses to assess safety concerns and accessibility issues.
Helpful Tip: Keep a written copy of all medications, dosages, and timing instructions from hospital staff. This documentation becomes vital when multiple carers are involved in daily care routines.
While this checklist helps, understanding how information actually moves between teams is just as important.
How Do Health Professionals Share Information During Transitions?
Health professionals share information through electronic discharge summaries, care plans, and direct communication with your GP.
In most cases, hospitals send discharge summaries electronically to your GP within 24 hours of release. These summaries include:
- Current medications
- Recent test results
- Instructions for ongoing treatment at home
- Contact details for care providers
- Emergency protocols and who to call after hours
In short, your GP receives everything they need to continue coordinating palliative care services without gaps. You should also receive paper copies of all medical information to share with home care teams or specialists if needed.
This dual system means both you and your doctor can access the same details, which reduces the risk of medication errors or missed appointments.
Managing Equipment and Medications at Home
Getting equipment and medications organised early means fewer stressful moments once your family member arrives home. So follow these steps to avoid unnecessary delays:
1. Medical Equipment Setup
Suppliers deliver hospital beds, oxygen tanks, and mobility aids directly to your home address. They can also advise on what continence aids or specialised mattresses might work best, depending on your family member’s physical needs.
After delivery, community nurses demonstrate how to use equipment safely and fix common issues like alarm malfunctions or oxygen flow adjustments.
Quick Tip: Keep supplier contact details accessible for urgent repairs or equipment replacements down the track.
2. Medication Plans and Supply
Medication plans outline what medications the person needs, when to take them, and how much. Your palliative care team adjusts pain relief dosages based on changing symptoms at home. If nausea, breathlessness, or other symptoms appear, they’ll also modify treatment plans to keep your loved one comfortable.
From there, pharmacists can organise dose administration aids that sort medications by day and time (no need to remember which pills go when). However, remember you should request at least three days of medication supply before leaving the hospital to avoid gaps.
But what happens when someone has a condition that keeps progressing over time?
What Happens When Your Loved One Has a Life-Limiting Illness?
Life-limiting conditions like advanced cancer, heart failure, or terminal illness require ongoing symptom management from both hospital and home care teams. Because of this, care transitions happen more frequently as health needs change throughout the illness journey.
The person might move between the hospital and home several times as symptoms shift or complications arise. And each move requires clear communication about what stage the illness has reached. This helps families understand what resources and guidance they’ll need at each point.
At some stage, health professionals adjust treatment goals to focus on comfort rather than trying to cure the illness (because quality of life becomes the priority).
Support for Paediatric Palliative Care Transitions
Paediatric care moves involve specialised children’s teams who understand the unique needs of young patients and their families. To make this happen, children’s hospitals coordinate with community paediatric specialists who provide age-appropriate care at home.
These teams arrange school liaison and respite care during hospital-to-home moves. They also connect families with grief counselling resources and support groups that target parents and children facing life-limiting conditions.
Did you know? Paediatric teams offer culturally sensitive support for Torres Strait Islander peoples and Aboriginal families going through sorry business and sad news.
At the end of the day, paediatric care focuses on maintaining quality of life while honouring each family’s cultural values and beliefs about death and dying.
When Should You Contact Your Palliative Care Team During the Dying Process?
It’s understandable if you feel uncertain about when to call for help. But your care team wants to hear from you whenever you have concerns. And frankly, waiting too long can make symptom management harder for everyone involved.
Reach out immediately if you notice these signs:
- Pain Medications Changes: Your team can adjust dosages or add different medications to keep the person comfortable at home.
- Breathing Pattern Shifts: These shifts often signal changes in the dying process that health professionals can help you understand and manage.
- Caregiver Overwhelm: Many family members struggle with the physical and emotional demands, and your team can connect you with additional resources or respite services.
- Uncertainty About Changes: If you’re worried about what happens next, ask for guidance about what physical changes to expect in the final days.
Still uncertain? PalAssist provides 24/7 phone support when you need advice or just someone to talk through what you’re experiencing.
You’re Not Alone in This Transition
Coordinating care between the hospital and home involves many steps, but you don’t have to handle everything by yourself. The health professionals, community services, and specialist teams working with your family are all committed to making this shift as smooth as possible.
After all, the emotional and practical challenges of caring for someone with a life-limiting condition can feel heavy at times. That’s exactly why support groups exist, and why services like PalAssist offer free access to registered nurses who understand what you’re going through during this difficult time.
If you need advice, emotional assistance, or just want to talk through your concerns about the dying process, you can reach PalAssist at 1800 772 273. You can also reach out through online chat or email whenever questions come up.
Disclaimer
This blog provides general health and product information for educational purposes only. It is not intended to diagnose, treat, or replace advice from your healthcare professional. Always seek guidance from your GP, nurse, continence advisor, or pharmacist regarding your individual needs. If symptoms persist or you’re unsure about product use, consult a qualified healthcare provider.
READ MORE: Alice Levine: The Multi-Talented Star Shaping British Media 2026